Periodontal disease, or gum disease, can be a serious condition with many ramifications for your oral health. However, it could also be harmful to your overall health.
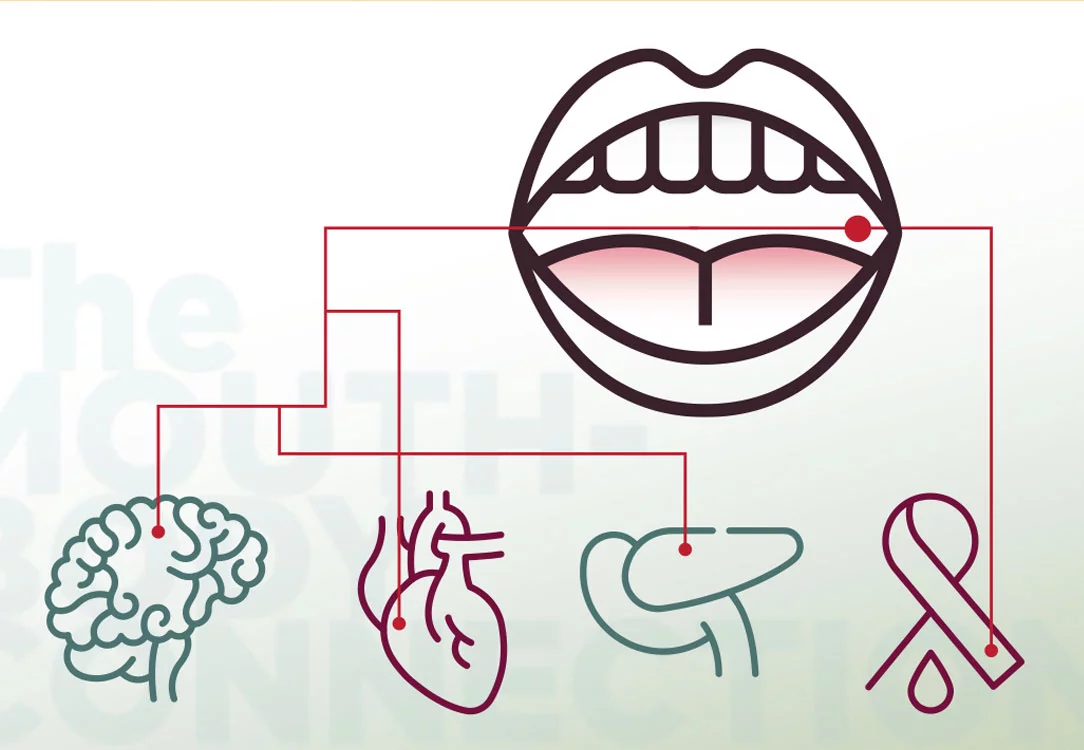
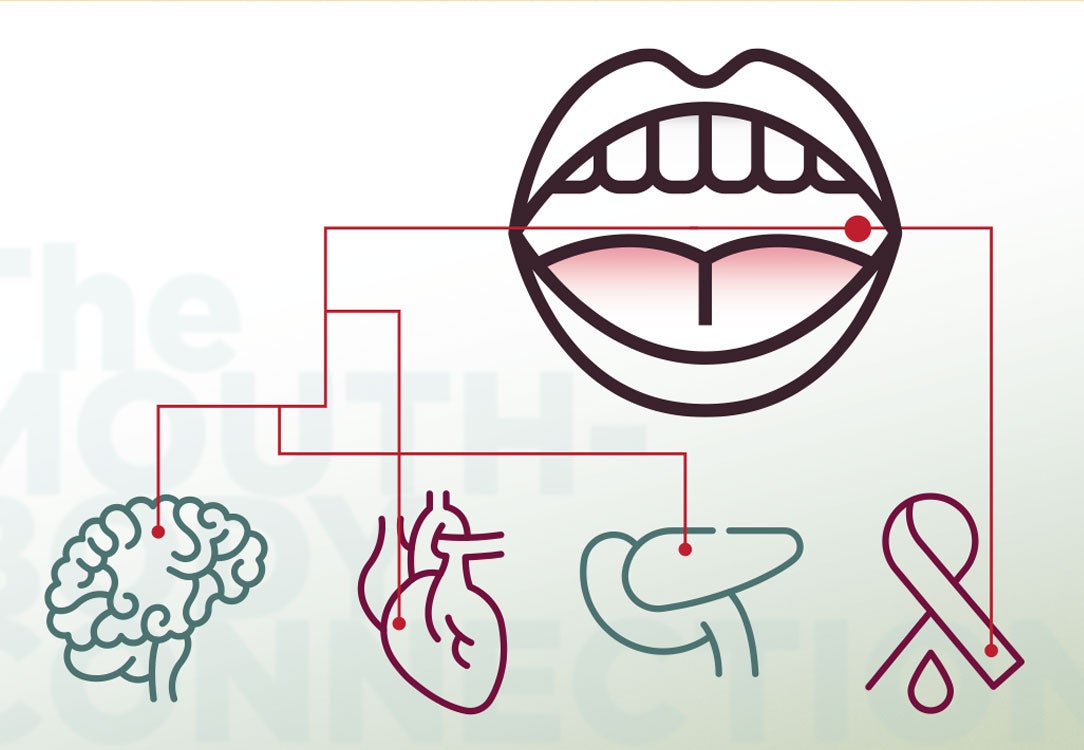
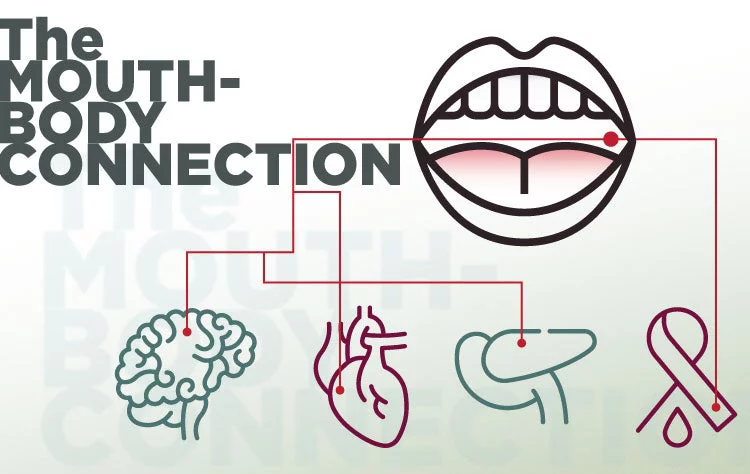
Gum disease is an integral part of the Mouth-Body Connection®, which is our term for how what's happening in your oral cavity affects what's happening in other parts of your body, too. The Mouth-Body Connection explains how the inflammation from gum disease can adversely affect the body's response to the management of other systemic conditions, particularly those that are also inflammatory. Gum disease is connected to serious conditions like cardiovascular and respiratory disease, strokes, Alzheimer's, rheumatoid arthritis, diabetes, and cancer, among others.
What is Gum Disease?
Common Risk Factors of Gum Disease
- Age: Older people are more likely to have gum disease than young people, especially those over 65.
- Smoking: Some studies show that tobacco use is one of the most significant risk factors for developing gum disease.
- Genetics: Some people are more prone to gum disease based on their heredity.
- Stress: Stress makes it harder to fight off infections like the one associated with gum disease.
- Medication: Some side effects from prescriptions you take can make your oral environment more susceptible to gum disease.
- Grinding Teeth: Patients who clench or grind their teeth can accelerate the development of gum disease resulting from the additional forces exerted on the teeth and supporting bone.
- Systemic Illness: Other inflammatory conditions can contribute to the progression of gum disease.
- Obesity: Extra weight is often indicative of a nutrient-poor diet, which inhibits the body's ability to fight off infection, placing you at a higher risk for severe gum disease.
Early Stages of Gum Disease
Gum disease has stages. The early stage of periodontal disease is gingivitis. However, if left untreated, gingivitis progresses to a more serious condition, periodontitis. Per the AAP, periodontitis is classified by stage and grade. The stage denotes the progression of the disease, and the grade communicates the rate of the disease progression and how the doctor thinks the infection will respond to treatment. [ii]
Early periodontal disease has many of the same symptoms as late-stage periodontitis, but the symptoms keep getting worse. More serious symptoms occur as the disease progresses through the gum disease stages. If you miss the early signs of gum disease, you could end up with a more severe form of the condition and face the loss of teeth and bone. For example, early-stage periodontitis has early gum recession. However, with moderate and advanced periodontitis, the gum recession worsens and leads to infection attacking the supporting bone, which makes your teeth feel loose.
Early-Stage Gingivitis
Gingivitis is the first stage of gum disease. It develops from plaque buildup, a combination of germs and bacteria that combine into a sticky substance, which is sometimes called biofilm. This biofilm hardens over time into calculus and tartar, which gather around your gum tissue. Tartar is challenging to remove from your teeth and is usually handled by your Smile Generation dental hygienist. As the tartar develops and increases, the buildup irritates the gums and creates the early stage of infection. Irritated gum tissue enables tooth decay to set in, also.
- Red gums
- Swollen gums
- Bleeding when brushing or flossing
- Gum tissue loss, called gum recession
- Bad breath
Early-Stage Periodontitis
- Red, inflamed gum tissue
- Swollen gums
- Gum recession with pockets of infection where the tooth and gum come together
- Bleeding when brushing and flossing
- Bad Breath
Moderate Periodontitis
- Same as early-stage periodontitis, only more severe, i.e., more bleeding and more gum recession
- Teeth feeling loose
- Beginning of supporting bone loss
- The inflammatory response in the body to the infection

Advanced Periodontitis
At this point in the progression of gum disease, the infection is getting severe. Some patients experience pain while chewing and their teeth feel loose in their mouth. Patients also have sores inside their mouths accompanied by bad breath and sensitive teeth. It is also the stage where a discharge of pus from the gums, called Pyorrhea, can occur. If left untreated, patients lose their teeth, and the infection will attack the jawbone.
- Swollen, tender gums
- Bright red, dusky red, or purplish gums
- More intense bleeding of gums, spitting out blood after brushing and flossing
- Persistent bad breath
- Pus discharge between your teeth and gums
- Loose teeth or tooth loss
- Pain while chewing
- Development of new spaces in teeth
- The appearance that your teeth look longer as gums pull away from teeth
- Changes to your bite, meaning the way the teeth come together
When Should I See My Dentist?
The good news is that you can stop the progression of periodontal disease. Early-stage gum infections can often be treated with improved and consistent home care. Often, diligent efforts to brush twice daily with fluoride toothpaste for at least two minutes, daily flossing, and using a medicated mouthwash can give your oral health the boost it needs to fight off infection.
We always want to see you here at your Smile Generation dental practice. However, we especially want to see you as soon as you notice early signs of gum disease. At the first sign of swollen gums or bleeding when you brush and floss, you should call your Smile Generation dental office and make an appointment, especially if you already have another chronic inflammatory disease diagnosis. When it comes to gum disease progression, the Mouth-Body Connection is clear inflammation in the body is not good for your gum disease and vice versa.
Find a Periodontist Near You
Millions of Americans have gum disease, and many don't know it. If you think you might be one of them, why risk the future of your healthy teeth and gums and the health of your body by avoiding the dental chair? Find a Smile Generation dentist here that can help. Treating gum disease today could save your teeth tomorrow.
Find your trusted, local dentist today!
Sources
[i] Gum Disease Risk Factors - American Academy of Periodontology. Perio.org. https://www.perio.org/for-patients/gum-disease-information/gum-disease-risk-factors/. Accessed April 1, 2022.
[ii] Gum Disease Information - American Academy of Periodontology. Perio.org. https://www.perio.org/for-patients/gum-disease-information/. Accessed April 1, 2022.
[iii] What is a Periodontist? - American Academy of Periodontology. Perio.org. https://www.perio.org/for-patients/what-is-a-periodontist/. Accessed April 1, 2022.
[iv] Gingivitis - Symptoms and causes. mayoclinic.org. https://www.mayoclinic.org/diseases-conditions/gingivitis/symptoms-causes/syc-20354453. Accessed April 1, 2022.
[v] Periodontitis - Symptoms and causes. MayoClinic.org. https://www.mayoclinic.org/diseases-conditions/periodontitis/symptoms-causes/syc-20354473. Accessed April 1, 2022.
[vi] Cafasso J, Frank, DDS C. Periodontitis: Symptoms, Causes, and Treatments. Healthline.com. https://www.healthline.com/health/periodontitis. Published 2017. Accessed April 1, 2022.
[vii] Cafasso J, Frank, DDS C. Periodontitis: Symptoms, Causes, and Treatments. Healthline.com. https://www.healthline.com/health/periodontitis. Published 2017. Accessed April 1, 2022.
[viii] Periodontitis - Symptoms and causes. MayoClinic.org. https://www.mayoclinic.org/diseases-conditions/periodontitis/symptoms-causes/syc-20354473. Accessed April 1, 2022.
[ix] Eke PI, Dye BA, Wei L, Thornton-Evans GO, Genco RJ. Prevalence of Periodontitis in Adults in the United States: 2009 and 2010. Journal of Dental Research. 2012;91(10):914-920. doi:10.1177/0022034512457373
Smile Generation blog articles are reviewed by a licensed dental professional before publishing. However, we present this information for educational purposes only with the intent to promote readers’ understanding of oral health and oral healthcare treatment options and technology. We do not intend for our blog content to substitute for professional dental care and clinical advice, diagnosis, or treatment planning provided by a licensed dental professional. Smile Generation always recommends seeking the advice of a dentist, physician, or other licensed healthcare professional for a dental or medical condition or treatment.